Transcranial magnetic stimulation (TMS) is a non-invasive brain stimulation treatment for various mental health conditions, such as major depression, obsessive-compulsive disorder (OCD), and anxiety. It can also address neurological disorders like Parkinson’s disease and chronic nerve pain. TMS uses magnetic fields to stimulate nerve cells in specific brain regions, improving mood regulation and cognitive functions.

"*" indicates required fields
We will get back to you in a few hours.
The efficacy of TBS is still being studied, but it has shown promise in treating a variety of conditions, including depression, OCD, bipolar disorder, and chronic pain. There is some evidence that TBS may be more effective than traditional TMS. Research shows that it can treat depression faster due to a shorter response time. For example, a study published in Molecular Psychiatry in 2024 evaluated six TBS protocols and found that they were more efficient and potentially more effective than TMS in reducing depression symptoms. Due to such research, TBS is becoming increasingly common as a treatment option. More and more insurance companies are starting to cover TBS, which makes it more accessible for people who need it.
Reduces Depression Symptoms
TMS is highly effective in reducing symptoms of depression. Patients receiving this treatment improve ... their mood, energy levels, sleep quality, appetite, and concentration. The effects can last 6-12 months after the completion of therapy.
Read moreNon-Invasive
Approach
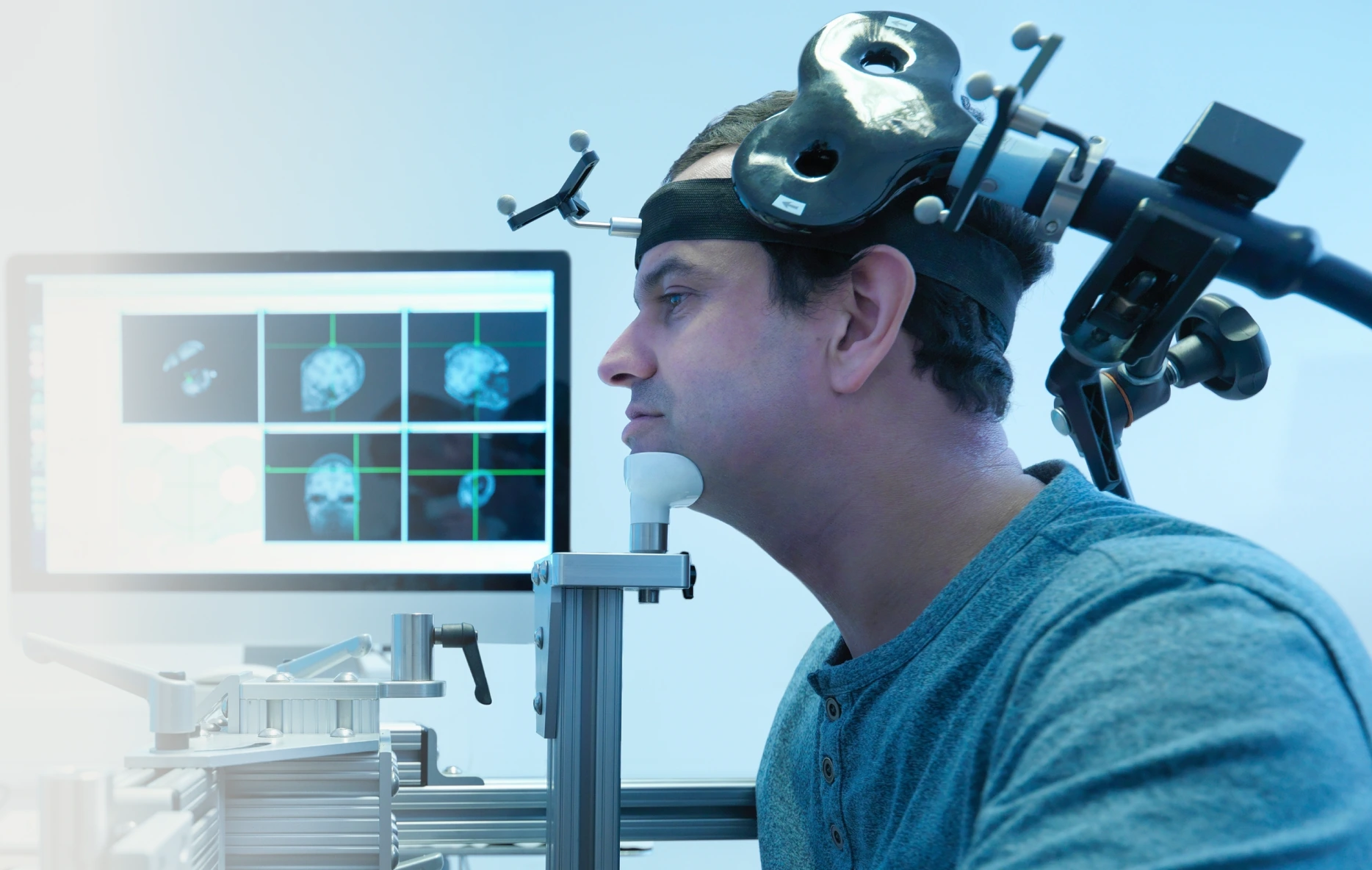
One of the major advantages of TMS over other depression treatments is that it is non-invasive. No surgery or... anesthesia is required. During a typical TMS session, the patient sits in a chair while a technician positions an electromagnetic coil near the scalp. The pulses that are generated can pass through the skull and stimulate nerve cells in the parts of the brain involved in mood regulation. The procedure is well-tolerated with few side effects.
Read moreSafe to Use
Numerous research studies have established TMS as a safe therapy. It does not disrupt brain structures necessary for thought, ... speech, movement, or memory. The most common side effect is a mild headache or scalp discomfort during or after the procedure. More serious risks are very uncommon if appropriate screening is conducted beforehand. This treatment is much safer than other brain stimulation therapies, such as electroconvulsive therapy.
Read moreRapid, Convenient Sessions
A standard course of TMS involves short daily sessions delivered five days a week for 4-6 weeks. Each appointment... takes less than an hour, and patients can return to regular activity immediately. This level of convenience and the relatively short duration of treatment are significant advantages over psychotherapy or medication, which may require a longer time commitment.
Read more